When a forensic pathologist performs an autopsy, one of the most critical steps is removing the brain. It’s not just about taking out an organ-it’s about preserving evidence, understanding trauma, and reconstructing what happened in the final moments of life. The way the brain is removed can make or break a case. In forensic settings, the goal isn’t to minimize damage like in surgery-it’s to collect complete, undistorted data. That’s why the occipital hinge technique has become the gold standard in modern forensic pathology.
Why Brain Removal Matters in Forensics
In a homicide investigation, a brain injury might be the key to proving cause of death. A fall, a blunt force trauma, or a gunshot wound to the head can leave subtle signs-bruising, bleeding, or shearing of nerve fibers-that only show up when the brain is carefully examined. If the brain is torn or crushed during removal, those clues vanish. That’s why traditional methods, which involved cutting through the dura mater and severing arteries and nerves in a haphazard way, are no longer used.
Forensic pathologists need to see how the brain sits inside the skull, how the membranes wrap around it, and how the blood vessels connect. They need to preserve the in-situ anatomy-the brain as it was in life. This is where the occipital hinge technique changes everything.
The Occipital Hinge Technique: A Game-Changer
The occipital hinge technique was developed specifically to solve the problem of destroyed anatomy. Unlike older methods that cut away large sections of skull and removed the dura completely, this method keeps everything intact. Here’s how it works:
- The body is positioned face down (prone), which gives better access to the back of the skull.
- A scalp incision is made from the forehead to the neck, and the skin and muscle layers are carefully peeled back.
- A craniotomy is performed-not all the way through the skull, but just deep enough to separate the outer bone layer (periosteum) from the inner dura. This prevents tearing.
- A narrow strip of bone is removed, starting at the pterion (near the temple) and extending back to just below the transverse sinus, a major vein at the base of the skull.
- The real innovation: a cut is made through the diploic layer of the occipital bone-the spongy middle layer-down to the foramen magnum, where the spinal cord exits. This creates a hinge.
- With gentle downward pressure on the occipital wedge, the bone folds open like a trapdoor, exposing the brainstem and cerebellum without cutting into them.
- The dura is cut around the brain, but one side (usually the temporal side) is left attached. This keeps the dura in place, preserving the natural relationship between brain and skull.
- The spinal cord is cut at C2, and the vertebral arteries are divided from back to front, not randomly.
The whole process takes about 45 minutes for an experienced pathologist. But the value isn’t speed-it’s preservation. Every cranial nerve, every artery, every fold of the dura remains untouched. This means pathologists can see exactly how trauma affected the brain’s surface, how blood pooled, and whether there were pre-existing conditions like aneurysms or tumors.
What Gets Preserved? The Anatomy That Tells the Story
With the occipital hinge, you don’t just get the brain-you get the whole package:
- Cranial nerves: The 12 pairs that control vision, hearing, swallowing, and facial movement. If one was crushed in a car crash, you’ll see it.
- Vasculature: The internal carotid, vertebral, and basilar arteries. Bleeding patterns here can show if trauma happened before or after death.
- Dura mater: The tough outer membrane. Tears or hemorrhages here can indicate rapid pressure changes, like from a blow to the head.
- Suboccipital triangle: A small space behind the skull where nerves and vessels cross. Damage here is rare in trauma but can reveal surgical interference or unusual force.
- Tentorium cerebelli: The fold of dura that separates the cerebrum from the cerebellum. Its integrity helps determine if the brain was compressed or displaced.
These structures don’t just help identify cause of death-they help reconstruct the sequence of events. A fracture in the occipital bone combined with a torn vertebral artery? That suggests a fall from height. A subdural hematoma with intact dura? That points to blunt force, not a stabbing.
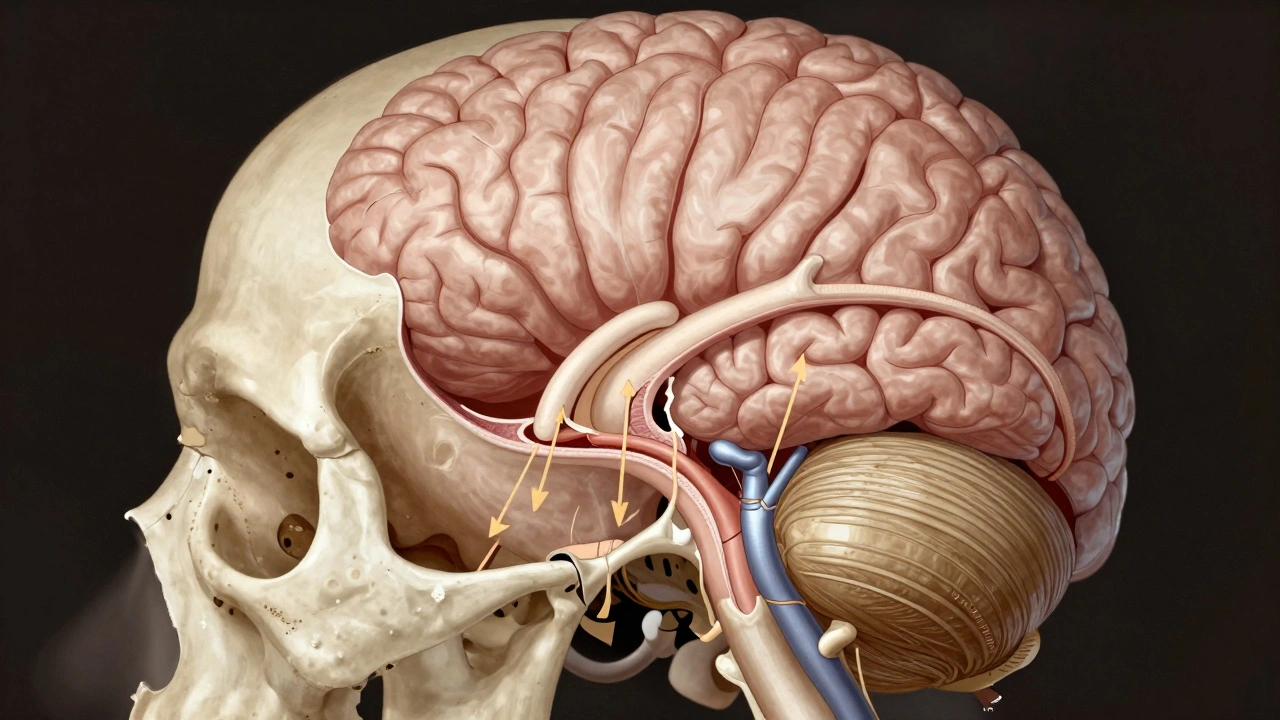
How It Compares to Old Methods
Before the occipital hinge, the standard method was the “circular craniotomy.” The pathologist would cut a full circle around the skull, lift the entire top off, then cut the dura away completely. The brain was pulled out by the brainstem, often tearing the cranial nerves and crushing delicate structures.
That method had one big flaw: it destroyed the very evidence pathologists needed. A torn nerve could look like trauma, even if it was caused by removal. A crushed artery might be mistaken for a hemorrhage. The dura was gone-so you couldn’t tell if it had been torn by injury or by force.
The occipital hinge fixes that. It’s not just safer-it’s more accurate. And in court, accuracy matters. A defense attorney will pounce on any sign that the autopsy was done carelessly. This technique removes that vulnerability.
Other Techniques You Might See (And Why They’re Not Used in Forensics)
In clinical neurosurgery, surgeons use techniques like keyhole craniotomies, endoscopic approaches, or awake brain surgery to remove tumors. These are brilliant for living patients-but useless in forensics.
- Endonasal endoscopic surgery: Uses a scope through the nose. Great for pituitary tumors. But it doesn’t let you see the whole brain. Irrelevant for autopsy.
- Stereotactic radiosurgery: Uses radiation. No tissue left to examine. No use in forensics.
- Awake brain surgery: Requires a conscious patient. Doesn’t apply to cadavers.
Forensic pathology doesn’t need to save brain function-it needs to preserve evidence. That’s why these clinical techniques aren’t adapted for autopsies. The occipital hinge is the only method that balances access with integrity.
Why Safety Isn’t Just About the Pathologist
Safety in brain removal isn’t about gloves or masks-it’s about preventing contamination and preserving chain of custody. The occipital hinge reduces the risk of accidental damage, which means:
- Less chance of misinterpreting injury patterns
- More reliable testimony in court
- Higher quality samples for toxicology
- Less need for repeat autopsies
When a brain is removed carelessly, it can lead to wrongful conclusions. A pathologist might mistake a torn nerve for a gunshot wound. Or miss a small subarachnoid hemorrhage because the brain was twisted during removal. Those mistakes can send innocent people to prison-or let killers walk free.
The occipital hinge technique reduces those risks. It’s not just a better way to remove a brain. It’s a better way to seek justice.
Training and Adoption
This technique is now taught in every major forensic pathology fellowship program in the U.S. and Europe. Medical schools that train future pathologists require students to perform the occipital hinge on cadavers before they’re allowed to assist in real autopsies. It’s become as standard as wearing gloves and using a scalpel.
Some labs still use older methods out of habit, but they’re the exception. The shift happened fast because the evidence was undeniable: cases reviewed with the occipital hinge technique had fewer disputes, fewer appeals, and more convictions based on clear pathology.
What Happens After Removal?
Once the brain is removed, it’s weighed, photographed, and examined in detail. The surface is inspected for contusions, lacerations, or hemorrhages. Then it’s sliced into sections-front to back, side to side-to look deeper. Toxicology samples are taken from the vitreous humor, the cerebrospinal fluid, and the brain tissue itself.
After examination, the brain is returned to the skull, or sometimes preserved in formalin. In some cases, especially when the death is under legal scrutiny, the brain is kept intact for future review. The occipital hinge makes this possible because the brain can be repositioned without damage.
Final Thoughts
Brain removal in forensic pathology isn’t a routine task. It’s a precision operation. The difference between a good autopsy and a great one often comes down to one thing: how the brain was taken out. The occipital hinge technique doesn’t just preserve anatomy-it preserves truth.
For pathologists, it’s not just about following a protocol. It’s about honoring the dead by giving their story the most accurate voice possible. In a world where evidence is everything, this technique ensures that voice is heard clearly.
Is brain removal always part of an autopsy?
Not always. In cases where the cause of death is clearly external-like a gunshot wound to the chest or a massive car crash with no head trauma-the brain may not be removed. But if there’s any suspicion of head injury, neurological illness, or unexplained death, brain removal is standard. It’s the only way to rule out internal damage that doesn’t show on the outside.
Can brain removal affect the appearance of the face during viewing?
No, not if done correctly. The occipital hinge technique leaves the skull intact, and the scalp is sewn back in place. The face, eyes, and jaw remain undisturbed. Families can have open-casket viewings without noticing anything unusual. Older methods that cut through the skull or removed large bone sections could distort facial features-this technique avoids that entirely.
How long does brain removal take during an autopsy?
With the occipital hinge technique, it takes about 45 minutes for an experienced pathologist. The entire autopsy usually lasts two to four hours, depending on complexity. The brain removal is one of the most time-consuming parts, but it’s also the most critical. Rushing it risks losing vital evidence.
Are there risks to the pathologist during brain removal?
The main risks are exposure to bodily fluids and potential needlestick injuries from sharp instruments. Pathologists wear full PPE-gloves, gowns, face shields, and sometimes respirators. The occipital hinge technique actually reduces risk because it’s more controlled and less chaotic than older methods. There’s no need to forcefully pull the brain out, which minimizes splashing or tearing.
Can brain removal detect drug overdoses or poisonings?
Yes. Brain tissue is one of the best places to detect certain drugs and toxins. Some substances, like alcohol, carbon monoxide, or heavy metals, accumulate in brain tissue and can be measured even after death. The occipital hinge technique allows pathologists to sample specific areas-like the basal ganglia or brainstem-where drug effects are most visible.