When a urine sample comes into a forensic lab, the question isn’t just whether someone used benzodiazepines - it’s which one, and when. The answer depends heavily on whether the drug was long-acting or short-acting. This isn’t just academic. In workplace testing, DUI cases, or overdose investigations, getting this wrong can mean misjudging someone’s responsibility, missing a pattern of abuse, or even misdiagnosing a medical emergency.
Why Duration Matters in Detection
Not all benzodiazepines are the same. Some stick around in your system for days - even weeks. Others clear out in hours. This difference isn’t just about how long the drug makes you sleepy. It’s about how long it shows up in tests. Long-acting benzodiazepines like diazepam and lorazepam have half-lives that can stretch from 30 to over 100 hours. That means if someone takes a single dose, the drug and its active metabolites can still be detected days later. In fact, with repeated use, these compounds build up in fat tissue and slowly release back into the bloodstream. That’s why a person who took diazepam on Monday might still test positive on Friday - even if they never took another pill. Short-acting drugs like alprazolam and triazolam are different. Their half-lives are typically 6 to 12 hours. They hit hard and fast, but they also leave fast. A single dose of alprazolam might only show up in urine for 1 to 3 days. That creates a narrow window for detection. If a test is done too late - say, 48 hours after use - you might get a false negative.What Gets Detected: Parent Drugs vs. Metabolites
Here’s where things get tricky. Most drug tests don’t just look for the original pill you swallowed. They look for what your body turns it into. Long-acting benzos like diazepam break down into multiple active metabolites: desmethyldiazepam, oxazepam, and temazepam. Each of these has its own detection window. Desmethyldiazepam, for example, can linger for up to two weeks. So even if the original diazepam is gone, the metabolite tells a different story - one that confirms long-term use. Short-acting drugs like alprazolam also metabolize, but their metabolites don’t last nearly as long. The main one, hydroxyalprazolam, clears in under 24 hours. That’s why a test done 36 hours after use might miss it entirely - unless you’re looking for the metabolite too. This is why older immunoassays often fail. Many only screen for a few common metabolites and can’t tell the difference between a one-time use and chronic use. A positive result for oxazepam could mean someone took lorazepam yesterday… or diazepam three weeks ago. Without more precise tools, you’re guessing.The Testing Methods: Immunoassays vs. Mass Spectrometry
Most workplaces and emergency rooms start with immunoassays. These are fast, cheap, and easy. But they’re also crude. Lateral flow strips and ELISA tests often rely on antibodies that bind to broad chemical groups. That means:- They can miss metabolites that don’t match the antibody profile
- They can’t tell diazepam apart from clonazepam
- They frequently give false negatives for glucuronidated forms - especially with lorazepam, which is mostly excreted as a glucuronide conjugate
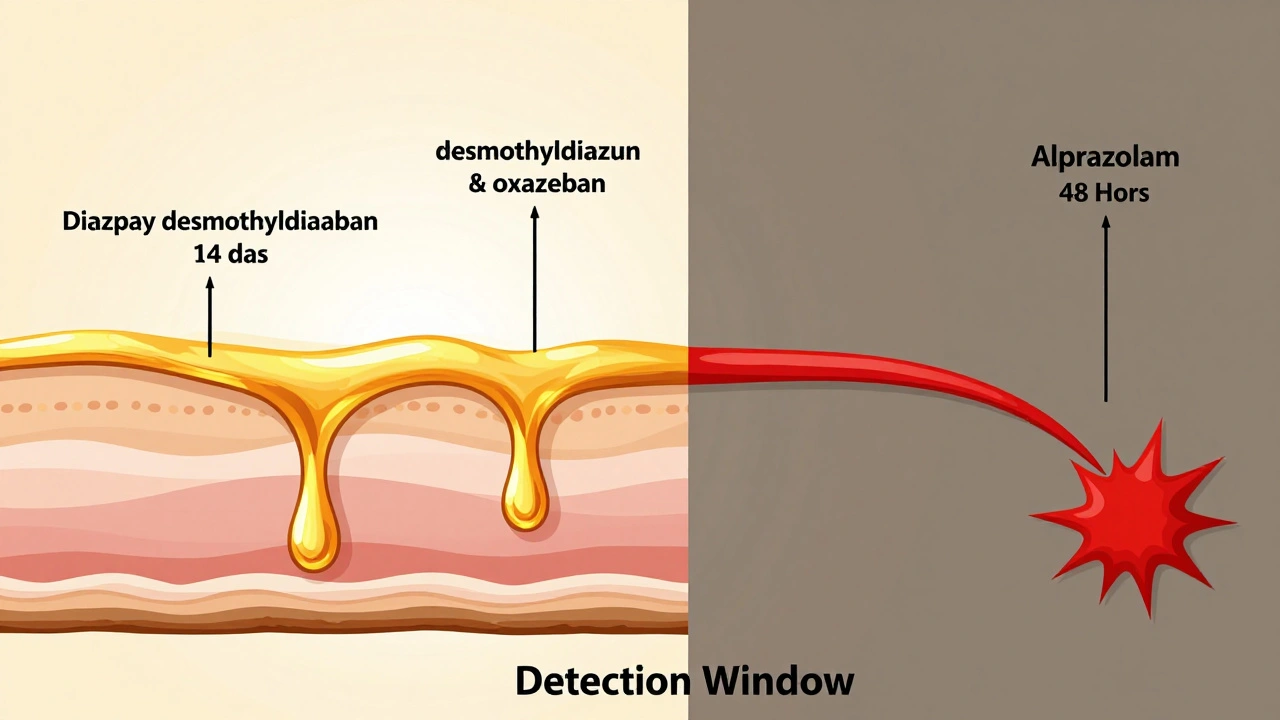
Detection Windows: What the Numbers Really Mean
Let’s cut through the noise. Here’s what actual studies show for typical urine detection windows under normal use:| Benzodiazepine | Type | Half-Life | Urine Detection Window | Key Metabolites |
|---|---|---|---|---|
| Diazepam | Long-acting | 30-100 hours | Up to 14 days | Desmethyldiazepam, Oxazepam |
| Lorazepam | Long-acting | 10-20 hours | 3-7 days | Lorazepam glucuronide |
| Alprazolam | Short-acting | 6-12 hours | 1-4 days | Hydroxyalprazolam |
| Triazolam | Short-acting | 2-4 hours | 1-2 days | None significant |
| Estazolam | Short-acting | 10-24 hours | 2-5 days | Desmethyl-estazolam |
The Glucuronidation Blind Spot
One of the biggest blind spots in traditional testing is glucuronidation. Many long-acting benzos, especially lorazepam and oxazepam, are excreted primarily as glucuronide conjugates - chemically modified forms that many immunoassays can’t recognize. This leads to false negatives. A person could have taken lorazepam the night before, but if the test doesn’t hydrolyze (break apart) the glucuronide bond, it won’t see the drug. That’s why some labs now use enzymatic hydrolysis before testing - turning the conjugated metabolites back into their free form so they can be detected. A 2022 study showed that one lab-developed test increased lorazepam detection by 30-fold after hydrolysis. That’s not a tweak - it’s a revolution in accuracy.What About Hair or Blood?
Urine is the standard, but it’s not the only option. Hair testing can detect benzodiazepine use over months - sometimes up to 90 days. But it’s not perfect. It’s expensive, sensitive to external contamination (like secondhand smoke), and can’t tell you when the drug was taken, only that it was used sometime in the past. Blood tests are better for detecting recent use - especially in acute cases like overdoses or DUIs. But they’re invasive, have a very short detection window (usually under 24 hours), and aren’t practical for routine screening. For most forensic and workplace purposes, urine remains the gold standard - but only if you’re using the right test.
False Negatives Are the Real Problem
In 2018, a study looked at reflexive testing protocols - meaning if an initial immunoassay came back negative, the lab automatically ran a more sensitive test. The result? False negatives dropped from 47% to just 2%. That’s not a minor improvement. That’s a game-changer. It means that for years, nearly half of benzodiazepine use cases went undetected because labs were relying on outdated, low-sensitivity methods. The shift isn’t just about technology. It’s about mindset. You can’t assume a negative result means no use. You have to ask: Which test was used? Was hydrolysis applied? Does it detect metabolites? Was the sample tested within the right time frame?What’s Next for Detection?
The field is moving fast. New methods like paper spray-mass spectrometry and DART-HRMS allow labs to test samples with almost no preparation. One study showed that a handheld DART instrument could detect benzodiazepines at airports with 97% accuracy - all in under 30 seconds. But the real breakthrough isn’t speed. It’s specificity. The ability to say: This person used alprazolam on Tuesday, not diazepam on Monday. That’s what matters in court, in treatment, and in safety evaluations. For now, the best practice is simple:- Use high-sensitivity immunoassays that account for glucuronidated metabolites
- Confirm all positives - and even some negatives - with GC-MS or HRAM
- Understand the pharmacokinetics of the drug in question
- Never interpret a negative result without knowing the test’s limitations





