Key Takeaways
- Histopathology looks at tissue architecture, not just individual cells.
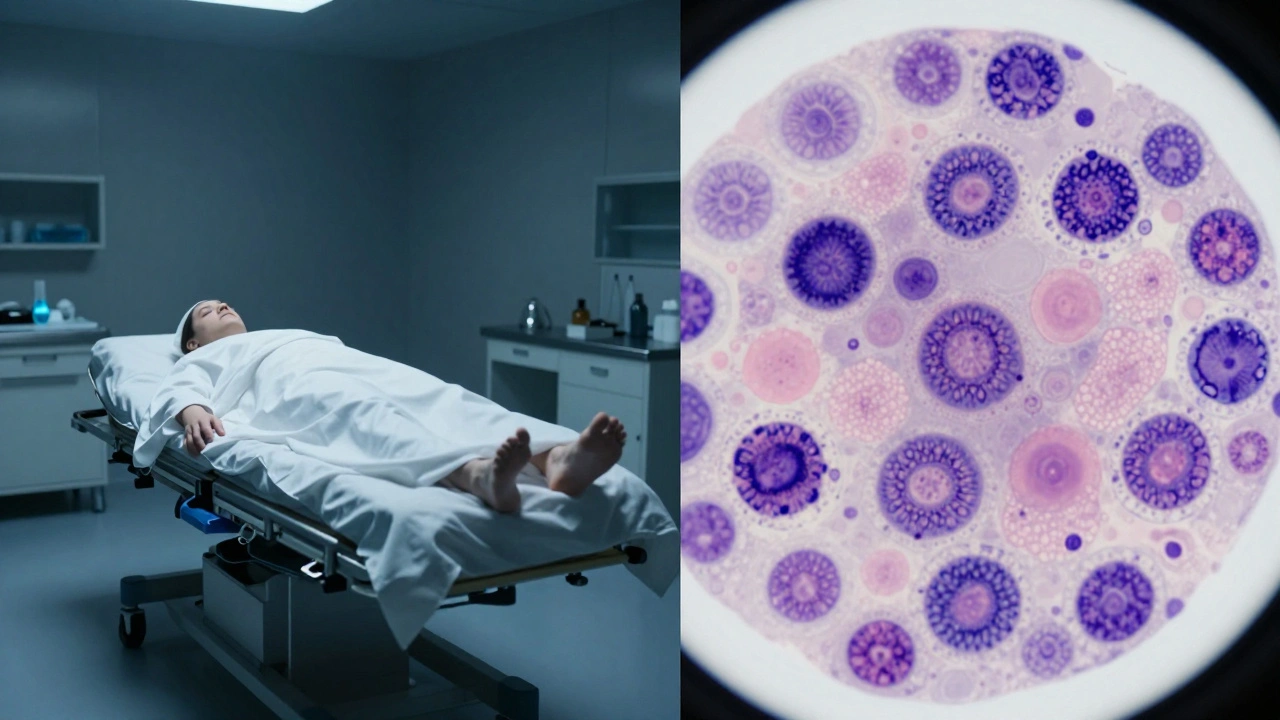
- The H&E stain is the gold standard for visualizing tissue structure.
- It is the definitive way to diagnose cancer and many systemic diseases.
- In forensics, it helps distinguish between natural death and foul play.
The Big Difference: Histopathology vs. Cytopathology
People often confuse histopathology with cytopathology, but they are very different tools in a doctor's kit. Think of cytopathology like looking at a few loose bricks from a building; you can tell if the bricks are cracked, but you don't know where they were in the wall. Cytopathology examines free cells or tiny fragments. Histopathology, on the other hand, is like looking at the entire wall. It preserves the "architecture" of the tissue. Because the cells remain in their natural organization, a pathologist can see if a group of cells is invading a neighboring area-a classic sign of malignancy. If you're trying to figure out if a tumor is benign or malignant, you need the structural context that only a tissue section provides.From Biopsy to Glass Slide: The Process
Getting a piece of tissue from a patient or a forensic subject to a microscope isn't as simple as just putting it under a lens. There is a rigorous, multi-step sequence required to keep the cells from rotting or distorting.- Fixation: The moment tissue is removed, it starts to break down. To stop this, it's placed in a fixative (usually formalin). This "freezes" the cellular structure in place.
- Embedding: Since tissue is soft and floppy, it's nearly impossible to slice thinly. The lab embeds the sample in Paraffin Wax, creating a hard block that can be sliced.
- Sectioning: Using a precision tool called a microtome, the technician cuts the wax block into slices so thin (often 4-5 microns) that light can pass through them.
- Staining: Most tissues are transparent. To see anything, they need color. The most common method is the H&E stain (Hematoxylin and Eosin). Hematoxylin turns nuclei blue/purple, and Eosin turns the cytoplasm and connective tissue pink.
| Method | Processing Time | Best Use Case | Trade-off |
|---|---|---|---|
| Paraffin Embedding | Hours to Days | Detailed cancer diagnosis | Slow turnaround |
| Frozen Section | Minutes | Intraoperative decisions | Lower image quality |
| Touch Preparation | Very Fast | Lymphoma screening | Crushes tissue architecture |
What Pathologists are Actually Looking For
When a Histopathologist-a medical doctor with specialized training-peers through the microscope, they aren't just looking for "bad cells." They are looking for specific morphological patterns. One common sign is necrosis, which is essentially cell death. In a forensic case, the pattern of necrosis can tell you if a heart attack happened minutes before death or if a toxin caused a slow organ failure. Then there's fibrosis, where healthy tissue is replaced by scarring. This often points to chronic disease or old injuries. In oncology, the focus shifts to dysplasia (abnormal cell growth) and neoplasia (the formation of a new, uncontrolled growth). The pathologist asks: Are the nuclei too large? Is the cell dividing too fast? Is the tumor pushing through the basement membrane into the blood vessels? These answers determine the stage of cancer and the treatment plan.
The Role of Histopathology in Forensic Investigation
In the world of Forensic Pathology, histopathology is often the final word in a "death mystery." While a gross autopsy looks at the whole organ, the microscopic exam reveals the invisible. For example, if someone dies of a suspected drug overdose, the organs might look normal to the naked eye. However, histopathology can reveal pulmonary edema (fluid in the lungs) or specific changes in the kidney tubules that prove the presence of a toxin. It's also vital for dating injuries. By looking at the inflammatory response-how many white blood cells have rushed to the site of a bruise or cut-a pathologist can estimate if an injury happened two hours or two days before death.Reading the Pathology Report
Once the analysis is done, the findings are compiled into a report. This isn't just a "yes or no" document; it's a detailed map of the tissue. A high-quality report typically includes:- Gross Description: What the tissue looked like to the naked eye (size, color, weight).
- Microscopic Findings: A detailed description of cellular changes, such as inflammation or malignant clusters.
- Tumor Margins: In surgical cases, the report specifies if the edges of the removed tissue are clear of cancer. If the margins are "positive," it means some cancer was left behind.
- Final Diagnosis: The professional opinion on what the disease is and its severity.
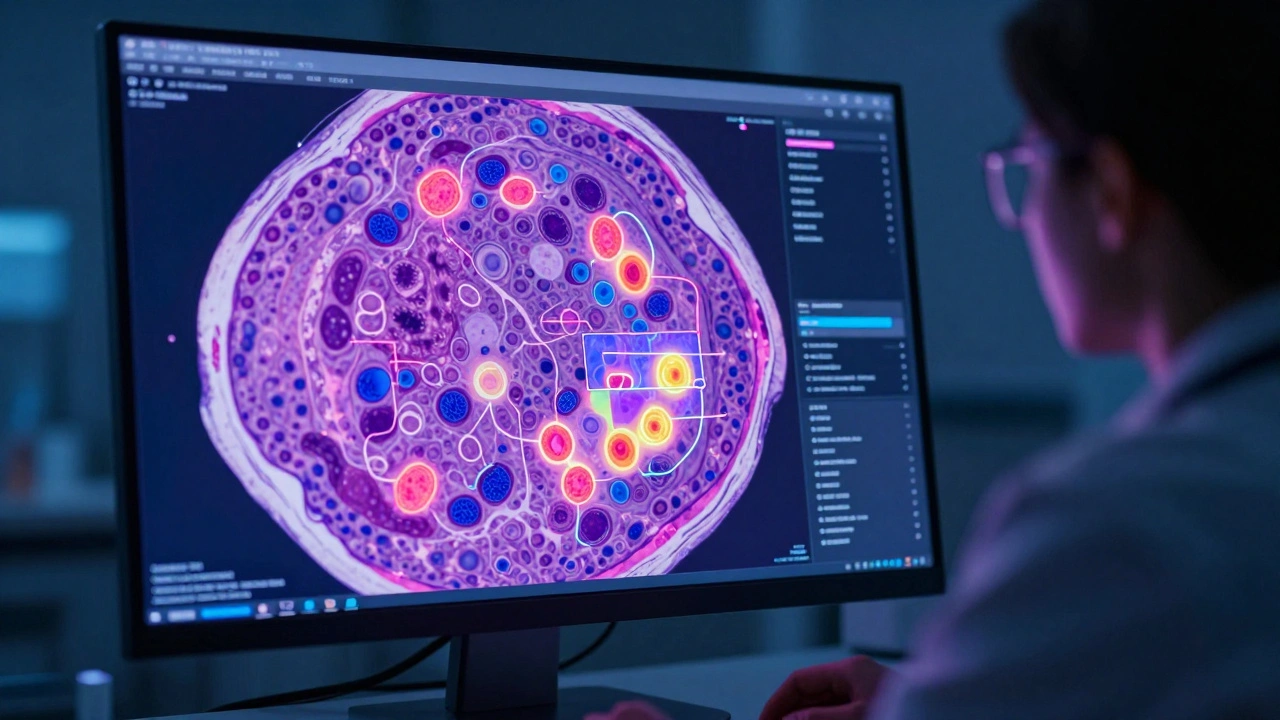
The Future: Digital Pathology and AI
We are currently moving away from the traditional "eyes-on-glass" approach. Digital Pathology involves scanning slides at incredibly high resolutions, turning a physical slide into a giant digital image. Why does this matter? First, it allows for remote consultation. A pathologist in Portland can send a digital file to a world-renowned expert in London for a second opinion in seconds. Second, it opens the door for AI. Machine learning algorithms can now scan thousands of cells to count mitotic figures (dividing cells) much faster and more accurately than a human ever could. This doesn't replace the doctor, but it gives them a powerful tool to ensure no tiny cluster of cancer cells is missed.Is histopathology the same as a biopsy?
No. A biopsy is the procedure used to *collect* the tissue sample. Histopathology is the *study and analysis* of that sample under a microscope after it has been processed in a lab.
Why is the H&E stain used so often?
It is the gold standard because it provides the best contrast between the nucleus (blue) and the cytoplasm/extracellular matrix (pink), allowing pathologists to see the general architecture and cellular detail of almost any tissue type.
How long does it take to get histopathology results?
Standard paraffin processing usually takes a few days because the tissue needs time to be fixed, embedded, and sliced. However, "frozen sections" can provide results in as little as 15-30 minutes during a surgery.
Can histopathology identify the cause of death in a forensic case?
Yes. It can identify things like myocardial infarction (heart attack), pulmonary embolism, or specific toxicological effects that are invisible during a standard physical autopsy.
What happens if the tissue is not fixed properly?
If fixation is delayed or done incorrectly, the tissue undergoes autolysis (self-digestion). This creates "artifacts"-distortions in the cells that can make healthy tissue look diseased or hide important diagnostic clues.
Next Steps and Troubleshooting
If you are a clinician or investigator waiting on results, keep these scenarios in mind:- Inconclusive Results: Sometimes the sample is too small (insufficient tissue) or the fixation was poor. In these cases, a re-biopsy or the use of specialized immunological stains (like IHC) may be necessary.
- Discrepancies: If the microscopic findings don't match the clinical symptoms, a "correlation meeting" between the surgeon, clinician, and pathologist is the best way to resolve the conflict.
- Urgency: For critical cases where a patient is on the operating table, always request a frozen section rather than a permanent paraffin section to get an immediate (though slightly less detailed) answer.